Abstract
Objectives
Respiratory motion during PET imaging introduces quantitative and diagnostic inaccuracies, which may result in non-optimal patient management. This study investigated the effects of respiratory gating on image quantification using an amplitude-based optimal respiratory gating (ORG) algorithm.
Methods
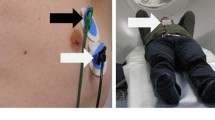
Whole body FDG-PET/CT was performed in 66 lung cancer patients. The respiratory signal was obtained using a pressure sensor integrated in an elastic belt placed around the patient’s thorax. ORG images were reconstructed with 50 %, 35 %, and 20 % of acquired PET data (duty cycle). Lesions were grouped into anatomical locations. Differences in lesion volume between ORG and non-gated images, and mean FDG-uptake (SUVmean) were calculated.
Results
Lesions in the middle and lower lobes demonstrated a significant SUVmean increase for all duty cycles and volume decrease for duty cycles of 35 % and 20 %. Significant increase in SUVmean and decrease in volume for lesions in the upper lobes were observed for a 20 % duty cycle. The SUVmean increase for central lesions was significant for all duty cycles, whereas a significant volume decrease was observed for a duty cycle of 20 %.
Conclusions
This study implies that ORG could influence clinical PET imaging with respect to response monitoring and radiotherapy planning.
Key Points
• Quantifying lesion volume and uptake in PET is important for patient management
• Respiratory motion artefacts introduce inaccuracies in quantification of PET images
• Amplitude-based optimal respiratory gating maintains image quality through selection of duty cycle
• The effect of respiratory gating on lesion quantification depends on anatomical location




Similar content being viewed by others
References
Bentzen SM, Gregoire V (2011) Molecular Imaging–Based Dose Painting: A Novel Paradigm for Radiation Therapy Prescription. Semin Radiat Oncol 2:101–110
Berghmans T, Dusart M, Paesmans M et al (2008) Primary Tumor Standardized Uptake Value (SUVmax) Measured on Fluorodeoxyglucose Positron Emission Tomography (FDG-PET) is of Prognostic Value for Survival in Non-small Cell Lung Cancer (NSCLC): A Systematic Review and Meta-Analysis (MA) by the European Lung Cancer Working Party for the IASLC Lung Cancer Staging Project. J Thorac Oncol 1:6–12
Bettinardi V, Picchio M, Di Muzio N, Gilardi MC (2012) Motion Management in Positron Emission Tomography/Computed Tomography for Radiation Treatment Planning. Semin Nucl Med 5:289–307
Bomanji JB, Costa DC, Ell PJ (2001) Clinical role of positron emission tomography in oncology. Lancet Oncol 3:157–164
Callahan J, Binns D, Dunn L, Kron T (2011) Motion effects on SUV and lesion volume in 3D and 4D PET scanning. Australas Phys Eng Sci Med 4:489–495
Carney JPJ, Townsend DW, Rappoport V, Bendriem B (2006) Method for transforming CT images for attenuation correction in PET/CT imaging. Med Phys 4:976–983
Chang G, Chang T, Pan T, Clark JW, Mawlawi OR (2010) Implementation of an Automated Respiratory Amplitude Gating Technique for PET/CT: Clinical Evaluation. J Nucl Med 1:16–24
Chen HHW, Chiu N-T, Su W-C, Guo H-R, Lee B-F (2012) Prognostic Value of Whole-Body Total Lesion Glycolysis at Pretreatment FDG PET/CT in Non–Small Cell Lung Cancer. Radiology 2:559–566
Dawood M, Buther F, Lang N, Schober O, Schafers KP (2007) Respiratory gating in positron emission tomography: A quantitative comparison of different gating schemes. Med Phys 7:3067–3076
de Geus-Oei L-F, van der Heijden HFM, Visser EP et al (2007) Chemotherapy Response Evaluation with 18 F-FDG PET in Patients with Non-Small Cell Lung Cancer. J Nucl Med 10:1592–1598
de Geus-Oei LF, van Laarhoven HWM, Visser EP et al (2008) Chemotherapy response evaluation with FDG–PET in patients with colorectal cancer. Ann Oncol 2:348–352
Dose Schwarz J, Bader M, Jenicke L, Hemminger G, Jänicke F, Avril N (2005) Early Prediction of Response to Chemotherapy in Metastatic Breast Cancer Using Sequential 18 F-FDG PET. J Nucl Med 7:1144–1150
Elmpt W, Hamill J, Jones J, Ruysscher D, Lambin P, Öllers M (2011) Optimal gating compared to 3D and 4D PET reconstruction for characterization of lung tumours. Eur J Nucl Med Mol Imaging 5:843–855
Erdi YE, Malawi O, Larson SM et al (1997) Segmentation of Lung Lesion Volume by Adaptive Positron Emission Tomography Image Thresholding. Cancer 12:2505–2509
Fletcher JW, Djulbegovic B, Soares HP et al (2008) Recommendations on the Use of 18 F-FDG PET in Oncology. J Nucl Med 3:480–508
Goerres G, Kamel E, Heidelberg T-N, Schwitter M, Burger C, von Schulthess G (2002) PET-CT image co-registration in the thorax: influence of respiration. Eur J Nucl Med Mol Imaging 3:351–360
Hoekstra CJ, Stroobants SG, Smit EF et al (2005) Prognostic Relevance of Response Evaluation Using [18 F]-2-Fluoro-2-Deoxy-D-Glucose Positron Emission Tomography in Patients With Locally Advanced Non–Small-Cell Lung Cancer. J Clin Oncol 33:8362–8370
Jani SS, Robinson CG, Dahlbom M et al (2013) A Comparison of Amplitude-Based and Phase-Based Positron Emission Tomography Gating Algorithms for Segmentation of Internal Target Volumes of Tumors Subject to Respiratory Motion. Int J Radiat Oncol Biol Phys 3:562–569
Korreman SS (2012) Motion in radiotherapy: photon therapy. Phys Med Biol 23:R161–R191
Mac Manus MP, Hicks RJ, Matthews JP et al (2003) Positron Emission Tomography Is Superior to Computed Tomography Scanning for Response-Assessment After Radical Radiotherapy or Chemoradiotherapy in Patients With Non–Small-Cell Lung Cancer. J Clin Oncol 7:1285–1292
Mikhaeel NG, Hutchings M, Fields PA, O'Doherty MJ, Timothy AR (2005) FDG-PET after two to three cycles of chemotherapy predicts progression-free and overall survival in high-grade non-Hodgkin lymphoma. Ann Oncol 9:1514–1523
Nehmeh SA, Erdi YE (2008) Respiratory Motion in Positron Emission Tomography/Computed Tomography: A Review. Semin Nucl Med 3:167–176
Nehmeh SA, Erdi YE, Pan T et al (2004) Four-dimensional (4D) PET/CT imaging of the thorax. Med Phys 12:3179–3186
Nestle U, Kremp S, Grosu A-L (2006) Practical integration of [18 F]-FDG-PET and PET-CT in the planning of radiotherapy for non-small cell lung cancer (NSCLC): The technical basis, ICRU-target volumes, problems, perspectives. Radiother Oncol : J Eur Soc Ther Radiol Oncol 2:209–225
Shankar LK, Hoffman JM, Bacharach S et al (2006) Consensus Recommendations for the Use of 18 F-FDG PET as an Indicator of Therapeutic Response in Patients in National Cancer Institute Trials. J Nucl Med 6:1059–1066
Weber WA (2005) Use of PET for Monitoring Cancer Therapy and for Predicting Outcome. J Nucl Med 6:983–995
Weber WA, Petersen V, Schmidt B et al (2003) Positron Emission Tomography in Non–Small-Cell Lung Cancer: Prediction of Response to Chemotherapy by Quantitative Assessment of Glucose Use. J Clin Oncol 14:2651–2657
Zaizen Y, Azuma K, Kurata S et al (2012) Prognostic significance of total lesion glycolysis in patients with advanced non-small cell lung cancer receiving chemotherapy. Eur J Radiol 12:4179–4184
Acknowledgments
The scientific guarantor of this publication is dr. E.P. Visser, Department of Radiology and Nuclear Medicine, Radboud university medical center, Nijmegen, The Netherlands. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. This study has received funding by Siemens Healthcare, The Hague, The Netherlands. This study was supported by an educational grant from Siemens Healthcare, The Hague, The Netherlands. The authors would like to thank James Hamill (Siemens) for scientific input. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was waived by the Institutional Review Board.
Methodology
Retrospective, experimental, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Grootjans, W., de Geus-Oei, LF., Meeuwis, A.P.W. et al. Amplitude-based optimal respiratory gating in positron emission tomography in patients with primary lung cancer. Eur Radiol 24, 3242–3250 (2014). https://doi.org/10.1007/s00330-014-3362-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3362-z